Candid Cancer: Progress has been erratic in the 40-year war on cancer
Editor's note: This is the first part of a series looking at the "war on cancer."
In 1971, President Richard Nixon signed the National Cancer Act into law and the war on cancer was on. Although neither he nor the legislation used the word war, it quickly became the metaphor used to describe the nation's campaign against cancer, a metaphor that implies the possibility of winning. In fact, Nixon charged scientists with winning — that is, curing cancer — by 1976, in time for the country's bicentennial.

As the Director of the University of Michigan Comprehensive Cancer Center, Dr. Max Wicha is a top general in the war on cancer.
University of Michigan
In these last 40 years, the federal government has spent $105 billion in its effort to fight the war, and others have contributed billions more. More than 2 million research papers have been published. And this year, the families of over half million Americans will cry at the funerals of loved ones lost to cancer — a number that equals one Twin Tower a day. It's not hard to see why some argue that we've lost the war.
But could something so complex as cancer, with all its variants, possibly be that simple? Or does understanding where we are in this war require understanding where we were when it began and then taking a broader view? To find out, I asked Dr. Max Wicha, director of the University of Michigan Comprehensive Cancer Center, who took time out of his extraordinarily busy schedule to share his vast insight.
We begin by getting comparisons to other achievements out of the way, comparisons, I learn, that are as irrelevant as comparing apples to oranges. Dr. Wicha lays to rest a question that's often asked: if we can put a man on the moon, why can't we cure cancer? "The difference," says Dr. Wicha, "is that we had all of the knowledge and all of the technology that we needed to get to the moon. Getting there was a matter of assembling all of the knowledge and the people who had the knowledge to put it all together in a very practical way."
And why, between 1975 and 2007, did the death rate from heart disease drop 64 percent while the death rate from cancer drop only 10 percent? Essentially, for the same reason we could put a man on the moon: the knowledge and technology most needed to solve heart disease was available early in the 20th century.
Conversely, neither technology nor knowledge capable of curing cancer existed in 1971. "The promise was made at a time that we didn't have the faintest idea of what cancer was," says Dr. Wicha, adding that it's impossible to conquer something when you don't know what it is you're trying to conquer. "It was naïve to think that we were going to cure cancer any time in the near future."
Dr. Wicha became an oncologist 10 years into the war, and even then, scientists still didn't know enough about the disease to make curing it possible. In fact, they barely knew that DNA was regulating cells. "If you'd asked me then what cancer was, I would have said that cancer is a disease where cells have abnormal growth, but that doesn't give you any clue of how you're going to attack it or cure it."
Without understanding the complexities of cancer, much less having the technology to unravel them, curing it quickly, then, was an unrealistic expectation, and unrealistic expectations lead to disappointment, and yes, criticism.
The reality was that without understanding the underlying cause of cancer, the best that doctors could do was treat the symptoms, which means treating it "essentially by trial and error," says Dr. Wicha. Physicians used techniques that were available — surgery, radiation and chemotherapy — "with somehow the hope that we'd come up with the right combination of things that were going to cure cancer. Again, I think that shows how terribly naïve we were."
Indeed, scientists didn't understand how or why chemotherapy worked, much less why it didn't. The era of chemical warfare on cancer began serendipitously in the 1940s when scientists discovered that mustard gas, a chemical weapon, could reduce tumors in patients with non-Hodgkin lymphoma. Other chemical drugs followed, all targeting one or more of the steps that lead to cell proliferation, but nothing explained why cancer cells proliferate.
Dr. Wicha tells me that in order to understand cancer, scientists had to understand not only the normal function of cells but also what tells them to grow, to stop growing, to make other cells. With that understanding, he says, "We now know that cancer is a fundamental abnormality of the makeup of how our cells function. Until we understood that, the idea of curing cancer was not only a fantasy but it was based on luck."
Dr. Wicha then tells me that some lucky things did happen. In some kinds of cancers, chemotherapy cured a substantial number of patients, even when the cancer was widespread. For example, when the war on cancer began, 90 percent of patients who got testicular cancer (think Lance Armstrong) died. Then, in 1974, a chemotherapy drug called cisplatin was combined with two other chemotherapy agents and the disease went from being nearly always fatal to one that was 80 percent curable.
Scientists didn't understand why the combination of certain drugs worked, but they pursued this approach which, at the time, seemed logical. After all, the history of medicine is replete with examples of scientists wandering down paths and stumbling on spectacular medical applications without understanding why they worked.
In retrospect, though, Dr. Wicha says of the early success of combining chemotherapy drugs, "It created, I think, an optimism that we were going to be able to do that for all kinds of cancers. Unfortunately, I think it led us down some blind alleys." He adds, "We spent 25 years or so taking different combinations of these agents, thinking that it was going to make a big difference." And did it? "We made a certain amount of progress because there were certain types of cancer that were sensitive to this approach, but they weren't the most common cancers."
But combining chemotherapy drugs wasn't all scientists were doing. They furiously attempted to develop other approaches, from vaccines to "magic bullets," drugs that would directly target the cancer. Along they way, technology improved and they discovered genes that trigger or promote cancer and genes that, when healthy, suppress tumors but when damaged, don't. Deeper and deeper they drilled into the mysteries of our cells and little by little, our cells gave up their secrets. But the death rate continued to climb with no cure in sight.
And then, in 1992, the mortality rate for all cancers in both men and women turned and has declined every year since, but the decline has been uneven. Between 1975 — the first year the National Cancer Institute (NCI) has solid, age-adjusted records — and 2007, the mortality rate for colorectal cancer dropped 40.5 percent; breast cancer, 27.4 percent; prostate cancer, 24.1 percent. The greatest declines occurred in the last 10 years, and they're largely attributed to screening for early detection, when cancers are more treatable, and to better therapies.
But the mortality rate in other cancers rose: melanoma, up 28.9 percent; kidney and renal cancer, up 10.8 percent (largely attributed to the rise in Hepatitis C); lung cancer, up 19.1 percent, although the mortality rate for this cancer peaked in 1993 and has since declined by 14.2 percent, thanks to a reduction in smoking. But these statistics are more than numbers: they represent real human beings, sobering reminders that this war is not over.
Still, there has been progress on a number of fronts. Among the 15 most commonly occurring cancers, the five-year survival rate has increased dramatically in most. While still low for liver, pancreas and lung cancers, 99 percent of men with prostate cancer now survive beyond five years as do 90 percent of women with breast cancer. And these days, newer treatments, for some cancers, are less invasive and/or disfiguring, and patients generally suffer less during treatment, thanks to discoveries that have helped to reduce side effects.
Indeed, researchers have been busy. Between 1971 and 2010, they published, according to the National Library of Medicine, 2,194,762 papers on cancer. Without a cure, the sheer volume has caused some to question if the quest for knowledge and the pressure to publish may have become an end unto itself rather than a means to an end.
Dr. Wicha clarifies how "the system" works, and I begin to see that this is not so simple as it seems on the surface. "Funding for research is very limited," he says, "and it's getting worse." He tells me that this year, only 7 percent of the grants that are reviewed by the National Cancer Institute (NCI) have guaranteed funding, and when competing for funding, published papers carry weight. "So if you don't publish those papers," says Dr. Wicha, "the chance of getting any money is nil." Not only that, funding is the currency of job promotion. Dr. Wicha and I agree that this may seem like a frustrating culture that doesn't directly do much for patients, but the fact is, we'd be a lot farther behind without all those papers. And indeed, some of them have resulted in significant changes in treatments and outcomes.
But elegant scientific papers can be published about discoveries made in a lab, only to be useless to patients if physicians can't apply the knowledge, and Dr. Wicha recognizes that there has been a gap between scientists and physicians. He explains that "the communication between them has been difficult because they work in two different worlds and even speak different languages." To help close the chasm, Dr. Wicha assembled groups of scientists and physicians who now work together — team science, he calls it. For patients, this team approach means that discoveries travel from the bench to the bedside faster.
For Michigan, it means research money, which ultimately benefits patients, too. Beaming, Dr. Wicha attributes this team approach as a significant reason why, this year, U of M topped all the medical schools in the country for NCI funding. He's rightfully proud. And so am I, but I also feel lucky that we locals don't have far to go to find cutting edge medicine when we need it.
Betsy de Parry
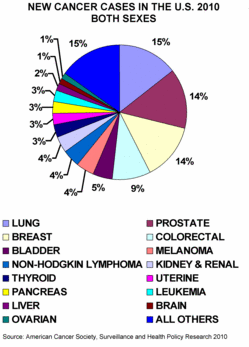
Funding, of course, has always been competitive, and there never seems to be enough. And let's face it. There are "have's" and "have-not's" in research funding and advocacy. Most of the attention and money goes to the most commonly occurring cancers, and the 15 most commonly occurring ones account for 85 percent of all cancers. What happens to the other 15 percent? In many cases, they're orphans in the worlds of both cancer research and advocacy, and they tell us another reason why progress has been uneven.
Take, for example, adrenocortical carcinoma (ACC), a rare cancer of the adrenal gland that claimed the life of Millie Schembechler, wife of Michigan's beloved football coach Bo Schembechler. Government funding for research has been almost nil. And many ACC patients don't respond well to the only drug available, a drug known as mitotane which is a derivative of the pesticide DDT and which was approved in — gulp — 1959, 12 years before the war on cancer began. No wonder the mortality rate has not changed significantly in 50 years. Only through the unrelenting efforts of U of M's own Dr. Gary Hammer, with funding by the only endowed professorship and research fund in adrenal cancer in the country, the first clinical trial testing a new treatment is now open.

So just where are we and where are we going in this war? Find out in part two of this report next Friday.
Next Friday, March 18: Victories are mounting in the 40-year war on cancer.
Betsy de Parry is the author of Adventures In Cancer Land and the producer of Candid Cancer reports for the PBS show A Wider World which airs in this area on Tuesdays at 5:30 on WTVS. Find her on Facebook or email her.


Comments
Val Shergin
Tue, Nov 15, 2011 : 6:20 a.m.
I'm sorry but have you not heard of Dr. Otto Warburg???? Dr. Otto Warburg finished one of his most famous speeches with the following statement: "…nobody today can say that one does not know what cancer and its prime cause is. On the contrary, there is no disease whose prime cause is better known, so that today ignorance is no longer an excuse that one cannot do more about prevention."[2] Otto Warburg won the Nobel Prize (in 1931 !!!!) for showing that cancer thrives in anaerobic (without oxygen), or acidic, conditions. In other words, the main cause for cancer is acidity of the human body. The cure is EASY. but there is NO MONEY to be made in "curing" it.