Taking the long view on health and habits, Ann Arbor program seeks to slash factors that lead to heart disease, diabetes
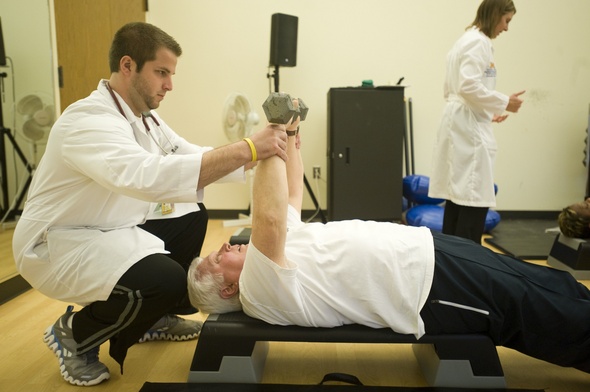
Exercise physiologist intern Ben Schelke helps Ann Arbor resident Frank Kurk with upper-body strength exercises last month during a metabolic fitness program at Domino's Farms Fitness Center.
Angela J. Cesere | AnnArbor.com
Frank Kurk, 67, has spent a lifetime on a weight roller coaster.
Diets have worked, and failed, and worked again for the retired Ann Arbor resident. But when Kurk's doctor discovered high blood sugar and blood pressure levels, plus an obese weight at an annual physical, Kurk decided the time for real change had arrived.
Kurk had metabolic syndrome, which means he has at least three of five risk factors that, left untreated, make the onset of cardiovascular disease or diabetes likely. The conditions open the door for heart attack, stroke and a host of other other costly and devastating complications.
According to the Centers for Disease Control and Prevention, one-third of adults in the U.S. have metabolic syndrome.
Factors for metabolic syndrome include central obesity, or gut fat; high triglycerides, meaning too much fat in the blood; low HDL — or “good” — cholesterol; elevated insulin while fasting; and high blood pressure. The condition afflicts millions of Americans, and its prevalence increases with age and a higher body-mass index.
Rather than hop on another diet bandwagon, Kurk enrolled in a metabolic fitness program offered at the University of Michigan Health System's Cardiovascular Medicine unit at Domino’s Farms. Stress, nutrition and exercise are among the topics addressed by a nurse practitioner, a behaviorist, a nutritionist and an exercise physiologist in the program, which entails weekly 90-minute sessions of education, discussion and exercise for either three or six months.
Melvyn Rubenfire, a preventive cardiologist at the University of Michigan, created the program in 2005. He’s quick to point out that a metabolic fitness program is not an obesity or weight loss program.
According to Rubenfire, the medical director for cardiovascular medicine for the U-M Health System, lifestyle changes are the best solution for metabolic syndrome, nipping in the bud factors that can lead to heart disease and diabetes.
These kinds of changes are challenging to manage for doctors crunched for time and for patients whose bad habits have become part of a comfortable daily routine.
But the metabolic fitness program makes an attempt.
“We look at people who are at risk, and we try to adjust those risk factors,” Rubenfire said.
Now, an article by Rubenfire and others on the 12-week version of the program is being reviewed by the Journal of Cardiac Rehabilitation and Prevention, he said.
It shows that the program eliminated metabolic syndrome in 20 percent of 126 participants enrolled between 2005 and 2009. The article seeks to show how a cardiac rehabilitation program can be adopted for managing lifestyle habits, which was the case at Domino’s Farms.
Soon, U-M will have data on more than 100 patients who have completed the newer six-month program. The results are promising so far. Forty-three percent of 63 people who have been tracked eliminated the condition via lifestyle changes taught in the course.
Blood sugar and triglycerides in particular take a dive for those who commit. Body composition changes for the better. And patients’ mental health tends to dramatically improve.
Successful participants are those who have resolved to change, Rubenfire said. For about one in five, the weekly lectures and exercise sessions make no difference whatsoever.
While the Washtenaw County Public Health Department doesn’t track metabolic syndrome among county residents, it does track obesity. Figures from the department's 2005 phone survey of 2,000 households showed that 18 percent of residents are obese, and nearly half of local residents are overweight. The survey is conducted every five years, but 2010 results are not yet available.
Rubenfire said those most at risk for metabolic syndrome would have someone in the family with diabetes, combined with the bad habit of eating lots of calories from foods with a high glycemic index, leading to gut fat. White bread is an example of such a food.
Almost six months after enrolling, Kurk has lost 80 pounds. He takes half the blood pressure medication he used to. His blood sugar is back within a normal range.
“Everything is better. Nothing is the same or worse,” Kurk said.
Kurk said he’s taken to heart what he’s learned during the program. The biggest lifestyle change has been with food. He used to eat out up to three times a day. Now, he eats out maybe once a week, exercises, and eats a lot more vegetables.
“I’ve learned how to think smarter when it comes to eating, and not just calories, but the balance of food and sodium levels,” he said.
At a recent session, he learned about strength training before working with a trainer on the exercises themselves.
The program is not covered by insurance, although blood work, a stress test and a medical assessment by a nurse practitioner at the start of the program typically are, said Rubenfire. Patients have to be referred to the program by a physician and it costs $350 or $700 for the three-month and six-month plan, respectively.
Rubenfire acknowledged many can’t afford the program. But he added that patients are more likely to attend, comply with what’s suggested and complete it if they pay. Rubenfire hopes to take the data he has collected to present it to some large corporations in Washtenaw County to see if employers will reimburse the cost of the sessions for their workers.
Kurk is convinced the program will pay off in more ways than one.
“There is certainly an expense, but if that expense equates to less medication and doctor visits down the road, then it will pay for itself,” he said.
Juliana Keeping covers general assignment and health and the environment for AnnArbor.com. Reach her at julianakeeping@annarbor.com or 734-623-2528. Follow Juliana Keeping on Twitter


Comments
REBBAPRAGADA
Sun, Apr 10, 2011 : 5:20 p.m.
Thanks for your response. I am speaking about the Law of Temperance as stated by poet John Milton in his epic poem of Paradise Lost. Angel Michael consoled Adam and had asked to observe the Law of Temperance and to simply avoid excess in what he eats and what he drinks. If Jesus doesn't work, we have to use the Natural Law of Temperance. It is all about being Smart in what we do.
REBBAPRAGADA
Sat, Apr 9, 2011 : 5:20 p.m.
Think smart while eating and drinking. The amount of food and beverages we consume are affected by the thoughts that we entertain as the thoughts formulate our eating behavior and the attitude towards food and drink. The smart way and attitude towards food is described in the Book of John, Chapter 6, verse 35. While eating food and while consuming liquids, man has to reflect on those ideas;"I am the bread of life. He who comes to Me shall never hunger, and he who believes in Me shall never thirst." We need to understand the mechanism that contributes to Satiation, the Satisfaction that is derived when man eats and drinks. This preventive approach is not adequate as it fails to define the term Health.
say it plain
Sat, Apr 9, 2011 : 5:59 p.m.
hey, whatever works for you ;-) We don't do the sorts of things day-to-day that people used to do, you know, back in the days of John and Jesus, like labor manually, get exercise, have limited food and drink. Now we drive everywhere and can buy food on credit cards and there's a for-profit food industry hoping we get addicted to Mountain Dew and potato chips... If appealing to the Lord Almighty helps some resist self-destruction via the chasing of temporarily-satisfying but ultimately-disease-inducing behaviors, then sure, why not? Some of us only need to feel the 'ick' of too much salted food and too many extra pounds on the belly, but I don't think that makes us morally righteous ;-)
say it plain
Sat, Apr 9, 2011 : 4:36 p.m.
Yes, @sh1, I agree that it's too bad such programs aren't covered by insurance. But so long as Big Pharma's lobbying arm can be so effective within our pay-to-play political system, diabetes drugs and high blood pressure medications win the day, *not* these lifestyle programs which truly bestow health instead of all the new symptoms and problems associated with the chemical dependences BigPharma prefers. Exercise is a better treatment for depression than pills are. But the people who might benefit from the pushing of exercise don't have lawyers in DC. So everyone's on psychoactive meds instead. The makers of drugs like Lipitor had physicians wondering whether they ought to just put statins in the water supply, they were so miraculous. Until it became clear that it caused all sorts of side effects that the drug companies actually knew about, but downplayed in their clinical reporting. It's more than a problem of "short-term profits", it's a question of *who* benefits from insurance's refusal to cover wellness programs.
sh1
Sat, Apr 9, 2011 : 4:03 p.m.
Sorry to hear the program is not covered by insurance. Too often, wellness plans are not covered in the goal to make short-term profits regardless of the long-term outcomes.