U-M study: Fear may be driving women to over-treat breast cancer
A new study conducted by the University of Michigan’s Comprehensive Cancer Center has shown that many women chose to over-treat their breast cancer because of unsubstantiated fears that it may return.
The study - released Tuesday night - revealed 70 percent of breast cancer patients that receive a double-mastectomy don’t have a clinical reason for having the procedure done.
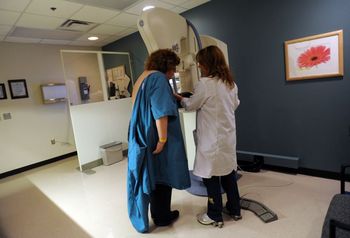
A woman receives a preventative screening for breast cancer. Researchers at the University of Michigan have found that many women with breast cancer choose to remove both breasts even though there's no clinical reason to do so.
Melanie Maxwell | AnnArbor.com
Researchers had observed a noticeable rise in the number of women that were choosing to have both breasts removed as a part of their cancer treatment strategy — a trend the team of Sarah Hawley, Steven Katz, Reshma Jagsi, all of the University of Michigan, suspected was due to more than just clinical attributions. Monica Morrow of the Memorial Sloan-Kettering Cancer Center, Ann Hamilton of the University of Southern California and Kendra Schwartz of Wayne State University also were authors of the study.
The study found 90 percent of women who had surgery to remove both breasts reported being very worried about the cancer recurring.
“There are women who are getting that procedure who could avoid it,” said Hawley, associate professor of internal medicine at the U-M Medical School and a lead author on the study. “Most women worry about (cancer) coming back.”

Sarah Hawley
Courtesy U-M
However, many women that do not have clinical reasons to remove both breasts choose to do so because they believe the procedure will reduce their risk for the cancer coming back, Hawley said.
“There is a significant proportion of women who don’t have the factors who are getting the procedure, and worry and concerns do drive some of these decisions,” Hawley said.
Hawley said it’s important to educate women that a contralateral mastectomy would not reduce the risk of cancer recurrence.
“Bilateral mastectomy does not reduce the risk of recurrence of breast cancer,” Sabel said. “There’s very little data that says removing both breasts will increase their chances of survival. The biggest threat to their survival is the cancer that they’re facing now. Most patients aren’t going to develop a second cancer.”

Dr. Michael Sabel
Courtesy U-M
For women who do not have a family history of breast cancer or cancer that has genetic mutations, they face the decision of whether or not they want to preserve their breast, which would involve the removal of the lump and radiation treatment, or if they want to remove the breast entirely.
“The outcome is the same,” Sabel said. “The survival of their cancer is no different whether they have breast preservation versus a mastectomy.”
Surgeons tend to favor less invasive treatments, Hawley said, and generally will recommend that women opt for the lumpectomy and radiation treatment if it applies to the patient’s situation, Hawley said.
Part of the confusion regarding breast cancer treatment is the cancer’s increased prevalence. Many women research treatment options online before talking with a surgeon, and many know other women that have gone through breast cancer treatments before, Sabel said.
“All it takes is one person to say, ‘I wish I had just had both breasts removed,’” Sabel said.
Misleading figures on many online resources overestimate the risk of breast cancer returning for a second time increasing at a rate of one to two percent per year, Sabel said. That figure is more like .2 to .4 percent, depending on how the breast cancer was treated the first time, Sabel said.
Especially for women in their 30s and 40s, they don’t want to undergo the breast cancer treatment process twice, Sabel said, and so many decide they simply want a double mastectomy when they don’t actually have a clinical reason for doing so.
“Some women fail to realize there can be complications,” Sabel said of double mastectomies. “Ten to 20 percent will have a complication unrelated to the cancer. People are overestimating the risk of cancer and underestimating the risk of the surgery.”
A double mastectomy has more risks involved because more anesthesia is required during the longer procedure. Recovery times also are longer, and reconstruction surgery becomes a much larger procedure if both breasts are removed.
Hawley stressed that even when both breasts are removed, a woman still needs to undergo chemotherapy treatments to prevent future activity by the cancer cells.
“One of the things that we believe and know from talking to a lot of surgeons that talk with us is sometimes these decisions get made too quickly,” Hawley said, explaining that women with breast cancer have the time to think over their options and don’t need to rush into the operating room that day.
Sabel said women have about a month to make a decision, even for patients with more aggressive forms of breast cancer.
The study was conducted using information from anonymous breast cancer patients registered in the National Cancer Institute’s registry, which has registered patients in the Detroit metro and Los Angeles metro areas. “Is Contralateral Prophylactic Mastectomy (CPM) Overused? Results from a Population-Based Study" will be presented at the American Society of Clinical Oncology Quality Care Symposium Nov. 30.
Hawley’s team is working to understand the general decision making process with regards to breast cancer treatment options. and has generated a number of studies using grant money from the National Cancer Institute.
The study conducted by Hawley’s research team serves as a natural segue into their next grant-funded project exploring patient values and concerns that lead to decisions regarding breast cancer treatment.
Using part of a $13.6 million National Cancer Institute grant, Hawley’s team will be working to develop an online interactive decision-making tool intended to help women diagnosed with breast cancer choose which course of treatment is best for them.
Amy Biolchini covers Washtenaw County, health and environmental issues for AnnArbor.com. Reach her at (734) 623-2552, amybiolchini@annarbor.com or on Twitter.


Comments
Narnia
Thu, Nov 29, 2012 : 11:04 a.m.
"A very small percentage of women who have breast cancer once will develop the cancer again, but most of them will be cured in the second round, Sabel said." This is completely false. If the cancer comes back, it has metastasized, and the prognosis is very poor. The National guidelines would then recommend palliative care. The only real breast cancer survivors are those whose death certificate lists a cause other than cancer.
David
Wed, Nov 28, 2012 : 8:57 p.m.
I wish that mental illness got this much attention!
DinaDarla
Wed, Nov 28, 2012 : 5:55 p.m.
Are you kidding me??? NEVER, EVER too much breast cancer awareness! I was JUST diagnosed very, very early only by virtue of going for my yearly mammogram each & every year at the same time-- and that would be with already knowing that I had a ZERO family history of breast cancer! ONLY because I was consistently proactive & totally insistent once receiving this recent & first questionable mammogram, did I even then switch to a true comprehensive & state of the art breast cancer center. Because of total breast cancer awareness my being aggressively proactive was I even diagnosed correctly & early! When you may be finding your self looking for excuses to put off or even skip your annual testing, please remember, my story. Breast Cancer Awareness is everything!! And-- all mammograms are not created equal! It truly makes a difference WHEN & WHERE you choose to go for your annual screenings!
dotdash
Wed, Nov 28, 2012 : 4:37 p.m.
It's that pesky difference between statistics that work for a population vs my life. I may know that a given treatment is just as good across the population, but since I only have my own life to gamble with, I may go for what seems like the surer option anyway.
RadicalBabe
Wed, Nov 28, 2012 : 5:10 p.m.
The risk of recurrence of breast cancer is higher than the risk of initial breast cancer in the general population. One in eight women will get breast cancer in their life. It is easy to manipulate statistics to prove whatever.
uabchris
Wed, Nov 28, 2012 : 3:48 p.m.
We are dealing with this now. What this story fails to say, is the survival stats are only for a 10 year window. If my wife was 80 this would be acceptable...my wife is in her 30s. Also my wife chose a little more surgery over more poison (radiation), which also has risks and complications. Additionally, its really hard to reconstruct one to match the other, thus you always have a visual reminder...these are just the conclusions we have arrived at after actually living this nightmare.
mady
Wed, Nov 28, 2012 : 7:12 p.m.
uabchris, prayers go out to your family.
thecompound
Wed, Nov 28, 2012 : 6:06 p.m.
Good points uabchris---and the very best wishes for your family :)
RadicalBabe
Wed, Nov 28, 2012 : 3:24 p.m.
The NCI reports no difference in survival rates, but they only report 5 year survival rates. Most women I know who had breast cancer died from recurrent breast cancer after they celebrated their 5 year survival. You can sometimes avoid chemo and radiation if you detect breast cancer early and opt for a double mastectomy. There have been recent studies that show chemo to be beneficial in the short run, but detrimental in the long run. As ObamaCare gets fully implemented, we can expect medical care options to be reduced for the majority as a means of providing cost savings to a medical system stretched to its capacity.
5c0++ H4d13y
Thu, Nov 29, 2012 : 11:33 a.m.
Jane unless all women are getting prophylactic bilateral mastectomy at birth they are all waiting to cross that bridge if it comes up. So once again. Healthy tissue is unrelated to recurrence.
jane
Thu, Nov 29, 2012 : 3:14 a.m.
5c0++ H4d13y - you don't want to "cross tat bridge when you come to it" because anyone that has endured nine months of chemo, surgery and radiation- would not want to risk having to do it again.
5c0++ H4d13y
Thu, Nov 29, 2012 : 2:47 a.m.
If I understand the article the point being made is that removing the other breast doesn't reduce the recurrence rate. How could it when the primary cancer didn't occur in the healthy breast. It may reduce the chance of a new cancer in the healthy breast but why not cross that bridge when ya come to it?
Robert Granville
Wed, Nov 28, 2012 : 2:43 p.m.
Maybe a little too much breast cancer awareness? I've been arguing this all year especially during the month. This is very similar to the recent discovery that healthy men should stop getting PSA blood tests to check for prostate cancer because it leads to unnecessary procedures and doesn't save lives overall. An oz of prevention, or in this case awareness, is not always worth a pound of cure.
justcurious
Wed, Nov 28, 2012 : 3:16 p.m.
I agree Robert. I wonder how much of this can be attributed to more money for the medical profession. While up north this last weekend we passed numerous pink dumpsters at the ends of drive ways. Companies have used breast cancer as a marketing tool it would seem, praying on the public's sympathies. It is to the medical communities monetary benefit to keep people scared.
Veracity
Wed, Nov 28, 2012 : 1:53 p.m.
Obviously, women with breast cancer need to be managed by capable breast cancer specialists who can educate their patients so that they choose appropriate care personalized for their cancers. Second opinions should be sought to confirm ideal management and for reassurance. Following this advice will hopefully reduce the frequency of unnecessary treatments.